My Return To Practice
6 June 2016 | Rebecca Myers

Rebecca Myers is a part time community staff nurse and executive coach/ organisational development consultant.
“We shall not cease from exploration, and the end of all our exploring will be to arrive where we started and know the place for the first time”
T.S. Eliot1989
I arrived early for my shift, and after a quick chat with the team on duty went to see Mary* – one of the patients I had been looking after – having been off for two days and keen to see how she was. Approaching her bed in the bay by the nurses’ station, I found the consultant ward round was taking place. Mary was showing signs of jaundice and clearly in discomfort. I could see the ascites she had was adding to her distress. She told me that the consultant was going to take her to theatre to insert a drain to remove the fluid. This would assist in alleviating her discomfort…
2016
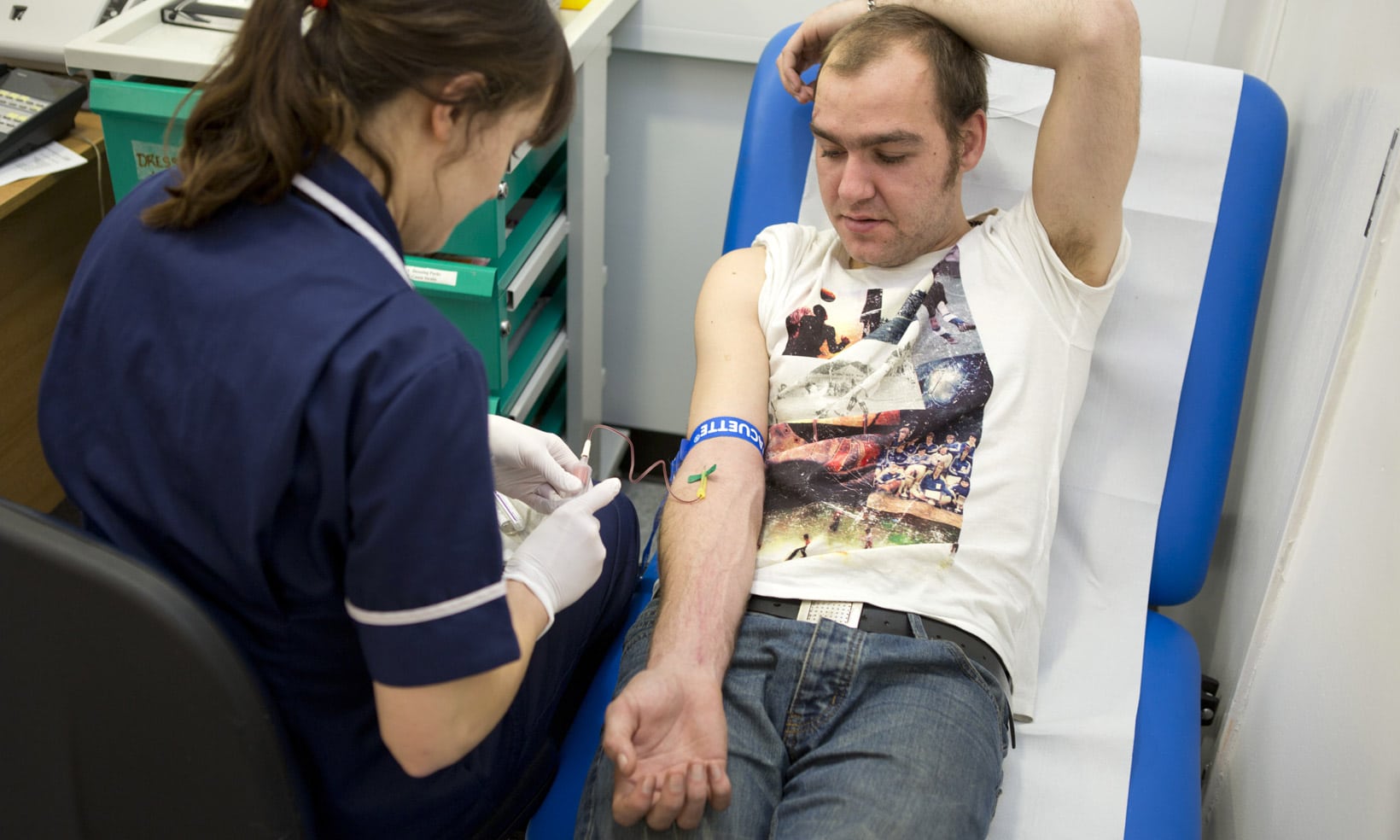
Fast-forward 25 years and here I am helping drain ascetic fluid from Jane’s* abdomen. Only this time, it’s not a bed in a bay, but a sofa in Jane’s living room. There is no team of doctors or nurses around, only myself, a colleague and an anxious relative. I’m very conscious of all the things that could happen: hypovolemic shock; sepsis; pain and distress or even respiratory or cardiac arrest. There is no high tech equipment or multidisciplinary team with us – they are a phone call away.
What we think and what is….
When I told people about returning to clinical practice after 25 years and wanting to work in the community, I received mixed responses including:
“That’s fantastic; I am not surprised’; “Don’t be ridiculous”; “You won’t be able to influence care as much as you do as a Director” and “ Why do you want to dress leg ulcers all day?”
It struck me how little the people I spoke to understood and appreciated what happened in community services and the knowledge and skills required to provide safe care in people’s homes. Even in the context of initiatives such as ‘hospital at home’ and ‘virtual’ wards set up by people like Sir Graham Morgan at Central Middlesex Hospital in London when I was working as a general manager in the mid 1990’s. In my time in hospital management, I would often describe how the general medical wards of those days were the High Dependency Units of my original nurse practice and now I find myself describing how the people we care for at home are the people we used to care for on the medical wards.
From managing chemotherapy, IV antibiotics, semi-acute exacerbations of respiratory and cardiac conditions, poly-pharmacy, post-operative and palliative care and interacting with colleagues in planning health and social care – to mention a few – or, as some have said, “people with leg ulcers”.
There are no cups of tea (although often offered) or cosy chats, but highly technical, complex interactions that are carried out whilst rapidly building trust and respectful relationships with ‘clients’, their families, carers and members of the wider Multi-Disciplinary Team (MDT) across the system of health and care.
The clients are either people who require a short intervention to regain independence and self-management, or those who have high levels of chronic need of health and social care; living in challenging, and at times, highly vulnerable circumstances.
Being in the client’s home changes the power dynamic; you are their guest and are able to see them as not just ‘someone with heart failure’ but a fellow human being who, just by the nature of their particular circumstances, is different to yourself.
For those who have spent many years working in this environment, I know I am not telling you anything you don’t already know; but with these changes happening over time, I wonder how often people step back and reflect just how much more responsibility and complexity community teams are dealing with now compared with 30 years ago. For those who haven’t ever worked in the community, or did many years ago, it may seem hard to believe and harder to appreciate the level of risk individual practitioners are managing.
Equipping people to do the role…
When I think about the work community teams now undertake (against the backdrop of proposed changes to nurse education and training) I believe the level of knowledge and critical analysis required to be a ‘good’ nurse is far greater today than when I trained 30 years ago. Although we studied anatomy and physiology with our medical student colleagues, our ability to put this into practice, in my experience, was often limited.
Too frequently others would say to me and my nursing peers: “That’s not for you to say/do/worry about as you are only the nurse”. This lack of ability to use my knowledge in caring for patients is one of the reasons why I left practice. Coming back I now see how application of this knowledge it is not only ‘allowed’, but critical if nurses are to provide the care that patients need. It is the situation today that nurses need to be trained at this level because they are saying, doing and worrying about these things, because they are the nurse.
Into the future…
So having started again as a community staff nurse, I am very conscious of ‘what I know’ and ‘what I know I don’t know’ (Burch 1970) and a sense of responsibility for providing the best care I can to people. I am very grateful for the support and supervision from the team which I have joined. Their knowledge, experience and wisdom is very present for me to draw on and not only enables me to return to practice but, more importantly, to provide excellent care to people who without that care would be back in those hospital beds with teams of professionals all around them.
* Names changed
References:
Burch, N. 1970 – Learning a New Skill is Easier Said than Done. Gordon Training International.

 Back to Blog
Back to Blog